What is Fetal Echocardiogram Ultrasound
During a fetal echo, an ultrasound probe is used to transmit and receive sound waves. This is similar to how an obstetric ultrasound is done. The test creates real-time, moving images of the fetal heart. It lets doctors view the heart, its blood vessels and the blood flow through the vessels and the heart’s four chambers.
Why Would I Need a Fetal Echocardiogram
A fetal echocardiogram is typically done when there is concern that the baby may have or is at higher risk to have heart disease.
Common reasons for performing a fetal echo include:
- Concern for a heart defect on obstetric ultrasound
- Parent or another child born with a congenital heart defect. (This is heart disease that is present at birth.)
- Suspected chromosomal abnormalities on prenatal genetic testing, (genetic testing before birth)
- Other fetal malformations seen on an obstetric ultrasound
- Maternal diabetes
- Irregularities in the fetal heartbeat
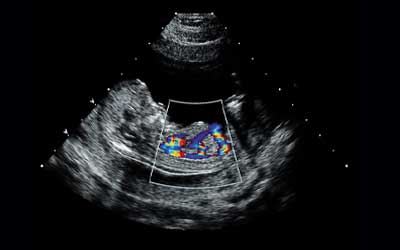
How Is a Fetal Echocardiogram Performed?
A fetal echo is painless. It is done like a regular obstetrical ultrasound. The pregnant mother must lie flat or on her side. This is sometimes uncomfortable for moms in late pregnancy.
You do not need to make any special preparations before your fetal echo. The test takes about 30 to 45 minutes. It is performed on an outpatient basis. You do not need to stay overnight for this test.
At Cincinnati Children's, a registered fetal sonographer does the echo. A pediatric cardiologist interprets the study. These heart specialists have advanced training in fetal imaging and cardiac ultrasound.
The test is done within our outpatient pediatric cardiology clinics. If abnormal, we will share the results with you immediately after the fetal echo is complete.
What Can Be Learned from a Fetal Echocardiogram?
A thorough fetal echo shows us the complete anatomy of the fetal heart. We can use it to assess heart function and identify normal or abnormal cardiac rhythms.
At What Stage of Pregnancy Should a Fetal Echo be Performed?
It is ideal for fetal echoes to be performed between 18-24 weeks' gestation (about mid-pregnancy). But they can be performed any time after this period.
Before 18 weeks of pregnancy, the small size of the fetus makes it more difficult to image the heart. However, in certain high-risk pregnancies, it is possible to complete fetal echoes as early as 12-14 weeks’ gestation.
When is the best time to do a HSG test procedure?How Will Information From the Test Be Used?
Information about fetal heart problems will be sent to your obstetrician and the pediatrician or neonatologists who would likely see your baby immediately following birth.
Some heart problems may need attention right away after you deliver your baby. The information from the fetal echo can influence the choice of where your baby should be born (high-risk obstetric center or a community facility). These test results also help us prepare how to care for the baby right after birth.
Some heart problems may be able to be treated before the baby is born. For example, for an unborn baby with an arrhythmia, we could give anti-arrhythmia medications to the mother during pregnancy.
Knowing about a potential heart problem before delivery gives a family a chance to learn more about the problem. This can help you prepare for handling the extra challenges you may face after birth. This may include surgery or other interventions your child might need. It also helps the medical team give the support and resources needed during your pregnancy to ensure the best possible outcomes at birth.
